India’s mental health crisis is worsening due to stigma, underreporting, and weak healthcare systems, leaving most people without treatment. Without stronger investment and awareness, it risks harming lives, productivity, and the country’s future growth.
Mental health is no longer a silent crisis; it is a raging epidemic whose signs are often ignored until it is too late. According to the WHO World Health Organization, mental health is a critical component of overall well-being, which enables people to cope with the stresses of life, realize their abilities, learn well, work productively, and contribute to their community.
An article by MedlinePlus states that mental illness is not caused by a single factor. There are many factors such as “feeling lonely” or “isolated”, “family history” and “genes”, “life experiences”, including “stress” or a “history of abuse” (including childhood abuse), “exposure to alcohol and drugs”, or even having a “serious medical condition” like cancer that leads to mental disorders. WHO also states that exposure to unfavourable circumstances, including “poverty”, “violence”, “inequality”, and “environmental deprivation”, also increases people’s risk of experiencing mental health conditions. Yet in India, it is still seen as “taboo, misdiagnosed, and systemic neglect”. In India, for the first time, while tabling the Economic Survey 2023-24, Smt. Nirmala Sitharaman, Union Minister of Finance and Corporate Affairs, talked about mental health, its significance, and implications on the country’s growth and cost. The cost due to mental Health is staggering.
Mental illness does not discriminate. It cuts across income levels, geographies, and age groups. It is shaped by a tangled web of social, economic, cultural, and environmental stressors, from poverty, caste discrimination, and gender violence to childhood trauma, academic stress, and job insecurity. For women, in particular, the impact of poor mental health is often compounded by social expectations, lack of autonomy, and limited access to care. Many experience undiagnosed postnatal depression or endure emotional abuse without any counselling support.
For the elderly, mental illness is often mistaken for age-related forgetfulness or isolation and dismissed without appropriate intervention. In the LGBTQIA+ community, rejection, marginalization, and fear of violence further escalate the risk of anxiety, depression, and suicide.
As per the National Mental Health Survey (NMHS) 2015-16, 10.6% of adults in India suffered from mental disorders. At the same time, the lifetime prevalence of mental disorders in India is 13.7%.
Notably, the prevalence of mental morbidity was higher in urban metro regions (13.5%) as compared to rural areas (6.9%) and urban non-metro areas (4.3%). Further, “15% of India’s adult population” requires active mental health care. Yet nearly 75% go untreated.” “Anxiety” and “depression” are the most common but often go unrecognized until they manifest in crisis, which mostly leads to “suicides”.
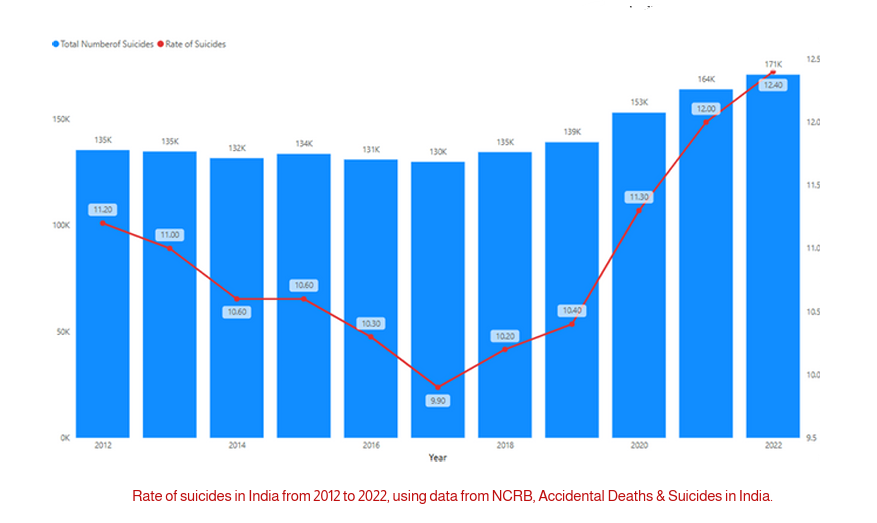
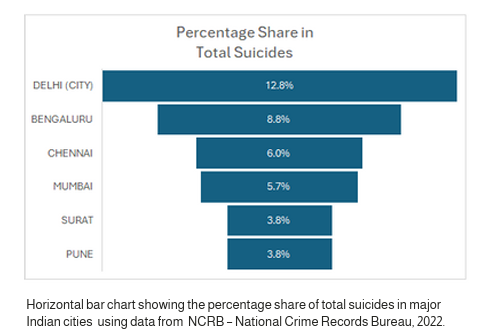
In India, Suicide rates have been rising. Over a decade, NCRB data shows a decline in suicide cases till 2017, but it increased from 10 per lakh in 2017 to 12.4 per lakh in 2022. Mental illness was the fourth leading cause, contributing to “8.5% of all suicide cases.” Yet this might “understate” the problem. Among the Indian states, Karnataka, Madhya Pradesh, Maharashtra, Tamil Nadu, and Punjab are the top five states with the highest indices of suicide influenced by mental illness. Altogether, they constitute 52.7% of total suicides determined by mental illness. Further, among cities, the metropolitan cities, Delhi, Bengaluru, Chennai, Mumbai, and Pune are reported as the top 5 cities with a 37.1% share in total suicide cases reported in 2022. This highlights these “dream” cities’ impaired pressure on population. the Further, working people between the age group of 18-45 years are more prone to commit suicide due to insanity/mental illness, as it was at 1 rank among causes of suicide of people aged 18-45, while it is at rank 2 for people aged 45 and above. Further COVID-19 pandemic also had a major impact on individuals’ mental health, as people struggled to cope with “social isolation”, “loneliness”, and “sudden loss of lives and livelihoods”. st Even people who don’t have a mental health condition may still face challenges to their mental health.
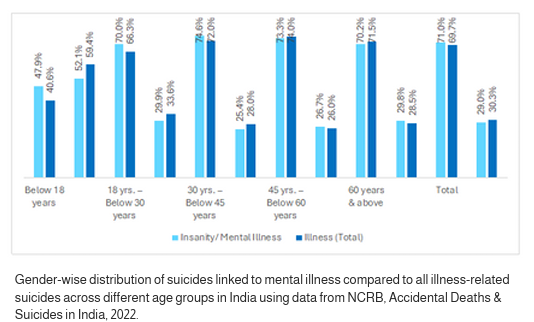
According to the Mental Health and Well-being of School Students Survey, the prevalence of poor mental health among adolescents was exacerbated by the COVID19 pandemic, with 11% of students reporting feeling anxious, 14% feeling extreme emotions, and 43% experiencing mood swings.
Therefore, it is being said that India’s demographic dividend is riding on skills, education, physical health, and, above all, the mental health of its youth. Though data in India shows an increasing trend of linkage of suicide due to mental health, yet this might understate the problem. WHO estimates that up to “90% of suicides” are underlying linked to mental health conditions. In India, suicide records often cite “family problems” or “illness,” glossing over the psychological distress beneath.
There is a “yawning gap between what is reported and what is real.” This data gap is particularly critical when designing national responses. Suicide prevention strategies must begin with a better understanding of root causes, and that requires better reporting, training of first responders, and community awareness. Today, families often record suicide under vague terms out of fear, stigma, or insurance denial. It perpetuates a cycle where policy fails to meet reality.
According to the Indian Journal of Psychiatry, India has “0.75 psychiatrists per 100,000 people”, far below the WHO recommendation of at least 3 per 100,000 people.
At the lower level, the condition worsens further, where families are left to navigate illness with no support or rely on traditional healers.
Many articles also state that individuals can experience “positive well-being” even if they are living with a “mental health condition”.
Even when services exist, quality is another challenge. A study by The Lancet (2020) showed that many mental health consultations in India are less than 10 minutes long, with little follow-up. In public hospitals, psychiatric wards are underfunded and overcrowded. Families bear the emotional and financial burden, often in silence. Public hospitals, burdened with high patient loads and constrained budgets, relegate psychiatric wards to overcrowded, poorly maintained corners of the facility. In the absence of government support, families shoulder not only the emotional trauma of caregiving but also the long-term financial costs. This often leads to cycles of silence, shame, and delayed or absent treatment, especially for women and children, whose symptoms are frequently dismissed.
Even in cities, mental health remains “taboo.” School surveys by NCERT reveal “43% of adolescents” experience mood swings, 11% report anxiety, and 14% struggle with emotional regulation.
Among adults, especially women, depression often presents as a physical illness and is rarely diagnosed. In workplaces, mental health is usually reduced to “token observances rather than systemic support.” Despite rising cases of burnout and work-related stress, very few consistent companies offer psychological counselling or stress audits. The Banyan, and iCall are building “community-based, lowcost” mental health care models. Startups like Wysa and MindPeers leverage digital platforms to reach younger, tech-savvy audiences.
Government efforts in recent years show promise but require strengthening. The National Mental Health Programme (NMHP) covers 767 districts through its District Mental Health Programme. The Mental Healthcare Act (2017) guarantees the right to mental healthcare and decriminalizes suicide. Tele-MANAS, launched in 2022, has handled over 1.8 million calls, offering multilingual counselling. Ayushman Bharat’s Health and Wellness Centres bring basic care to the grassroots. Yet mental health receives less than 1% of the total health budget.” Without substantial investment, such reforms risk remaining ‘symbolic.” Progressive states like Kerala, Tamil Nadu, and Delhi are implementing school counselling programs. NGOs such as Sangath, The Economic Survey 2024-25 recommends strengthening school mental health education, improving workplace policies, and expanding AI-enabled digital services. India stands at a crossroads. If mental health continues to be viewed as a “fringe issue,” we will continue to lose lives, productivity, and human potential. Mental health must be integrated into every governance layer, from schools and workplaces to panchayats and PHCs. It must be treated not as a luxury, but as a “basic right.” India has laid the foundation for a mental health revolution from TeleMANAS to school counselling, but without real investment, these steps risk becoming symbolic gestures. Mental health must move from the margins to the mainstream, treated as a basic right, not a luxury. Otherwise, we will keep losing lives, futures, and human potential to silence and neglect.
Clear Cut Health Desk
New Delhi, UPDATED: April 29, 2026 09:00 IST
Written By: ANJALI BANSAL and MOHITA BANSAL




