HPV vaccines can prevent up to 90% of cervical cancer when given early, offering strong protection against high-risk HPV strains. Early vaccination combined with screening provides the best defense against the disease.
Key Highlights
- HPV vaccines offer very high protection against persistent HPV infection and precancerous lesions.
- Studies show vaccination can reduce invasive cervical cancer by nearly 90% when given early.
- Single-dose schedules show up to ~97.5% efficacy against high-risk HPV strains.
- Vaccination combined with regular screening offers the best protection.
- Universal HPV immunisation remains critical for cervical cancer elimination strategies.
Human Papillomavirus (HPV) vaccines now have strong scientific evidence supporting their role in preventing cervical cancer and related diseases. International research, supported by decades of real-world data, shows that HPV vaccination dramatically reduces infection rates and precancerous changes that lead to cancer.
In simple terms, HPV vaccines train the body’s immune system to fight off the virus strains that most often cause cervical cancer. When given before someone becomes exposed to HPV — typically in adolescence these vaccines can prevent the infection that eventually leads to cancer. Health experts worldwide recommend vaccinating young people early in life, along with regular cervical screening for adults, to maximize protection and save lives.
What Is HPV and How Does It Cause Cancer?
Human Papillomavirus (HPV) is a group of viruses transmitted primarily through intimate skin-to-skin contact. Of the many strains, some (notably HPV-16 and HPV-18) are classified as high-risk because they can persist and transform normal cells into cancerous ones over time. Persistent infection with these high-risk types is the main cause of cervical cancer.
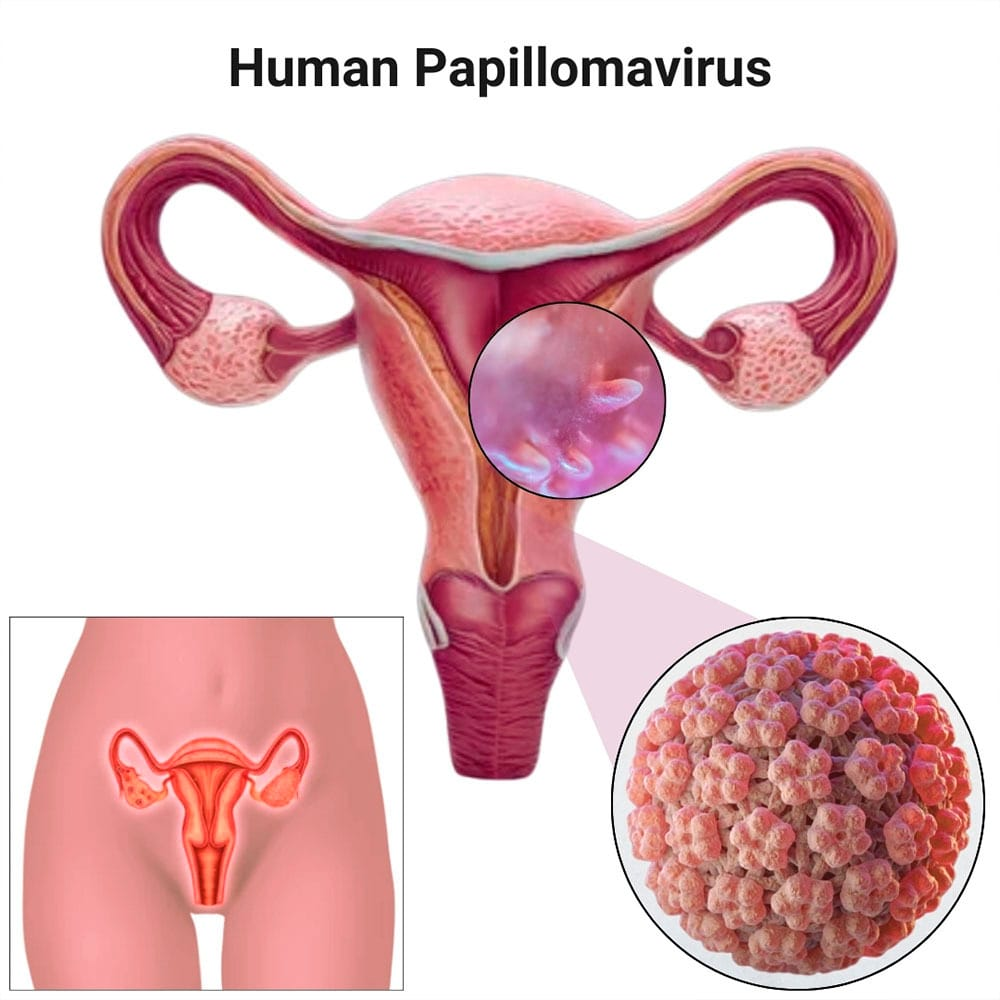
Cervical cancer remains one of the leading causes of cancer death among women globally, especially in low- and middle-income countries where routine screening and early detection services are less available. Persistent infection with high-risk HPV types accounts for the vast majority of cervical cancer cases.
How Effective Are HPV Vaccines?
Multiple global studies demonstrate exceptionally high vaccine efficacy:
- The Centers for Disease Control and Prevention (CDC) reports that HPV vaccines have close to 100% efficacy in preventing persistent infection with vaccine-covered HPV types and precancerous lesions in individuals not previously exposed to the virus.
- Large population research found that giving the HPV vaccine at ages 12–13 was associated with an 87% reduction in invasive cervical cancer and up to 97% decline in high-grade precancer lesions later in life.
- Randomized studies in Kenya and Costa Rica showed ~97.5% protection against the most dangerous HPV strains (16/18) after a single vaccine dose.
- Review evidence from systematic trials confirms that vaccination cuts the risk of developing cervical cancer by up to 80% or more when administered early.
This strong data shows that HPV vaccines not only prevent infection but also interrupt the progression from virus exposure to precancer and cancer.
Timing Matters: Why Early Vaccination Works Best
Medical experts agree that timing significantly affects vaccine effectiveness. Vaccination is most successful when delivered before an individual is exposed to HPV through intimate contact.
For this reason, health organisations recommend routine immunisation for:
- Girls and boys from around 9–14 years of age
- Catch-up vaccination for older adolescents and young adults who missed earlier doses
Vaccination schedules typically involve two doses for younger adolescents, while older groups may receive three doses. There is also growing evidence that a single-dose schedule may provide high and lasting immunity, simplifying delivery and reducing cost barriers.
HPV Vaccines and Global Public Health Goals
The World Health Organization (WHO) has set ambitious goals for cervical cancer elimination. The strategy includes:
- 90% HPV vaccination coverage of girls by age 15
- 70% screening coverage of women by ages 35 and 45
- 90% access to treatment for cervical disease and cancer
Achieving these targets could dramatically reduce new cervical cancer cases over the coming decades. However, vaccine coverage remains uneven: many low-income countries still have limited access to HPV vaccines and routine screening services, despite high cervical cancer burdens.
Safety and Real-World Impact
Extensive safety monitoring supports the vaccines’ favorable safety profile. Millions of doses administered globally show no serious long-term side effects directly linked to the vaccine.
Real-world studies tracking HPV vaccination programmes have also shown so-called herd immunity effects: infection rates fall not only in vaccinated individuals but also among unvaccinated people as overall virus circulation drops.
This makes the vaccine an effective public health tool beyond individual protection.
Beyond Cervical Cancer
While cervical cancer is the most prominent HPV-related disease, HPV vaccines also protect against other cancers caused by high-risk HPV types, such as:
- Anal cancer
- Vulvar and vaginal cancers
- Oropharyngeal (mouth and throat) cancers
These additional benefits strengthen the case for broad vaccination strategies.
The Social Dimension: Awareness, Access, and Equity
Cervical cancer disproportionately affects women in poorer communities. Lack of awareness, limited healthcare access, and social stigma around HPV — a sexually transmitted infection — often hinder vaccination uptake.
Public education must clarify that the HPV vaccine is a cancer prevention tool, not a commentary on behaviour. Health authorities and community organisations play a key role in dispelling myths and improving acceptance.
Wider vaccine availability, especially in low-resource settings, requires policy commitment and adequate funding. Many countries are integrating HPV vaccines into national immunisation programmes to make them free or subsidised — a step toward equitable health protection.
Vaccination and Screening: A Combined Approach
While HPV vaccination dramatically reduces cancer risk, it does not protect against all HPV strains or eliminate the need for routine screening. Pap smears and HPV testing remain vital for early detection in women of screening age.
Combining vaccination with regular screening maximises prevention and ensures early treatment where needed.
Conclusion
HPV vaccines represent one of the most powerful tools in modern cancer prevention. With high efficacy, long-lasting protection, and real-world evidence of dramatic reductions in cervical cancer risk, vaccination offers hope for eliminating a disease that still causes substantial suffering worldwide.
Understanding the science, improving access, and addressing social barriers are essential to protect future generations. Vaccination, coupled with routine screening, can save countless lives and transform women’s health globally.
Clear Cut Health Desk
New Delhi, UPDATED: March 03, 2026 09:00 IST
Written By: Samiksha Shambharkar




